All Features

Mike Morini
Following the turmoil of the pandemic, many salaried employees have had the opportunity to work remotely and enjoy newfound flexibility in their day-to-day work lives. For many, the ability to be more in control over where and when they work has been life-changing, enabling them to find better work…

Silke von Gemmingen
Rigid endoscopes are used in medical diagnostics and therapy to examine body cavities and hollow organs, and to perform minimally invasive procedures. To avoid risks for patients and medical staff, it’s essential that the devices function perfectly. Reliable quality testing is intended above all to…

Melissa Phillips
The levels of contaminants in our food supply are, generally, decreasing. That’s the good news.
But we still need to measure those contaminants and make sure our food is safe. And measuring tiny things (and big things) is what we do best here at NIST.
In our food safety program, we’re studying all…
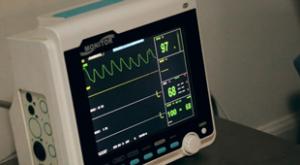
Etienne Nichols
Medical device companies must have established risk management processes that comply with ISO 14971. It doesn’t matter whether you’re developing medical devices in the U.S., EU, Canada, or elsewhere. Every international regulatory agency you’ve ever heard of accepts ISO 14971.
ISO 14971 is a good…

Ophir Ronen
From the health histories of patients to the effectiveness of different healthcare services, hospitals are sitting on a treasure trove of historical data. Unfortunately, most of these data go unused, often because they are so difficult to store or format for actionable use.
Due to inconsistencies…

Martin Cottam
It’s tempting to attribute the increased profile now given to occupational health and safety (OH&S) to the Covid-19 pandemic. But while in many organizations the pandemic shone a spotlight on OH&S management, there are other issues that will keep OH&S at the fore throughout the next…

Matthew M. Lowe
Change of any kind often requires a catalyst. This is particularly true in a business environment where the rule of thumb is to do things the way they’ve always been done. And when you’re working in a regulated industry, processes tend to get more locked in because compliance is at stake.
That was…

Michael Glickman
Artificial intelligence (AI) is revolutionizing the healthcare industry by enhancing decision-making capabilities, improving quality of care, and reducing costs. In the age of supercomputers and technological advancement, the health sector generates vast amounts of data, which AI can process and…

Kari Miller
Life science organizations depend on quality management systems (QMS) to improve products, minimize risks, ensure patient safety, and support regulatory compliance. When companies use a horizontal QMS that is not purpose-built for the life science industry, they must execute additional steps to…

Etienne Nichols
I have a bold opinion: The corrective and preventive action (CAPA) process is the second-most important component of your quality management system (QMS). (If you want to know what I think is No. 1, shoot me an email.) As you build medical devices, a well-defined CAPA program provides a framework…

Grant Ramaley
As of 2023, more than 27,000 medical device QMS certificates have been issued worldwide, providing confidence in medical devices. From cardiac stents to simple dental tools used to correct teeth, the healthcare systems of the world have come to rely on ISO 13485 to provide critical support to world…

Donald J. Wheeler, Al Pfadt
In memory of Al Phadt, Ph.D.
This article is a reprint of a paper Al and I presented several years ago. It illustrates how the interpretation and visual display of data in their context can facilitate discovery. Al’s integrated approach is a classic example not only for clinical practitioners but…

Etienne Nichols
On Dec. 9, 2022, the U.S. Food and Drug Administration (FDA) issued a new draft guidance, “Content of Human Factors Information in Medical Device Marketing Submissions,” that provides recommendations for the inclusion of human-factors information in marketing submissions.
The drafted guidance is…

Trupti Dhere
The healthcare industry is known for rapidly adopting advanced technologies that offer improved treatment for various diseases. Consequently, digital twin technology in healthcare has gained popularity during the past few years, owing to the range of advantages it offers.
Digital twin technology…

Etienne Nichols
In a highly regulated industry like medical technology, manufacturing processes must undergo either process verification or process validation to ensure they’re consistently producing the correct result. The question is, which one should you use?
Verification and validation are two different…

Liza Dzhezhora
Having appeared in the early 2000s, connected health technologies have gradually become a game changer in the healthcare industry. Healthcare providers that have embraced smart medical IoT solutions reduce costs, improve patient experience, and ensure preventive care.
The trend is not fading away…
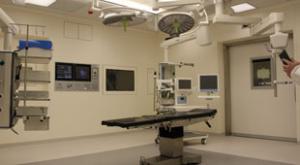
Scott Trevino
Nearly a quarter of surveyed healthcare cyberattack victims experienced increased mortality rates following a data breach, and more than half reported poorer patient outcomes due to longer hospital stays and delayed procedures. Healthcare has faced the highest average data breach cost—more than $10…

Amy Brown
Listening to customers is critical for healthcare organizations to ensure they’re delivering high-quality care to their patients. Sure, the traditional methodology of doing so via surveys can increase customer retention and profitability. But much like evolving from analog to digital, there’s a…
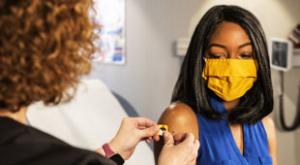
Gleb Tsipursky
One of the key stakeholders in stakeholder capitalism is the employee. You could argue that the employee is the key stakeholder, because without employees you’d have no stakeholders at all. This is why employers need to stay aware of today’s health environment and its effect on their employees.…

In a press statement released on Jan. 6, 2023, the European Commission reported the adoption of a proposal to allow more time to certify medical devices to mitigate the risk of shortages. The proposal introduces a longer transition period to adapt to new rules, as foreseen under the Medical Devices…

Bhushan Avsatthi
The very nature of healthcare construction and its specific infrastructural and functional needs pose significant challenges to the architectural, engineering, and construction (AEC) sector. Crucial hospital spaces such as operation theaters and critical care centers need fail-proof connections to…

Angie Basiouny
In the hustle of a busy hospital emergency department, teams of doctors and nurses react quickly to determine whether a patient needs to be admitted, referred, or released. Providing such complex care requires a high degree of skill and seamless teamwork, the kind that usually comes from years of…
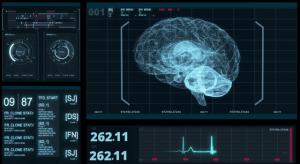
Doug Folsom
Unpatched vulnerabilities remain a target of cyberattacks, and an ever-present risk for healthcare organizations. Medical devices pose an additional burden because patches are frequently unavailable for medical devices. So, dealing with the potential threat isn’t usually straightforward. The stakes…

Dirk Dusharme
In 2010 a medical device scandal in France set the stage for a new European Union medical device regulation that, according to most experts in the medical device community, may cause more damage than the problem it was intended to address. An unreasonable deadline, lack of notified bodies to…
Alex Waddell, Diki Tsering, Peter Bragge, Paul Kellner
Emergency medical workers, already at increased risk for burnout compared to other professions, continue to be challenged by the fallout of Covid-19.
Stretched to the breaking point by increased workloads, highly contagious and acutely ill patients, and limited resources, workers’ risk factors for…