During the past year, my email inbox has been consistently pinged by law firms advertising seminars and workshops that promise to help medical professionals understand what is noteworthy for 3D-printed medical products, ranging from regulatory to IP concerns. Some of these have been quite alarming, seeming to indicate that as disruptive as 3D printing promises to be, there must be a corresponding disruption to how we work on regulatory compliance to protect our assets.
|
ADVERTISEMENT |
But if we step back and look at the actual U.S. Food and Drug Administration (FDA) communications, the pace of adoption of 3D printing and real intersections of 3D printing and business processes, it appears that little has changed. The only disruption is when 3D printing revolutionizes a commercial process.
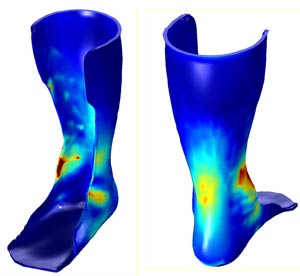
Image 1: Orthotic ankle support scans
…
Add new comment