Increasingly, the health care industry is benefiting from ISO 9000 and other quality systems. Such processes promote continuous quality improvement with a minimal incursion into caregivers' time. Improving management systems and operational processes is critical to providing customers with quality service. It's no secret that insurance companies, customers and other payers tend to do business with stable health care organizations; if they are ISO 9000-qualified, they will find that other survey processes prove much simpler and less costly. The following discussion of ISO 9000 in health care will help organizations working toward integrated health care quality management. Four broad groups within the industry will find advantages in implementing an ISO 9000 quality system:  Institutional health care providers -- This group consists of hospitals, medical centers and clinics that currently comply with standards set by the Joint Commission on Accreditation of HealthcareOrganizations. Compliance to JCAHO standards enables institutional health care providers to obtain Medicare reimbursement for services to Medicare patients. The Medicare system is administered by the Federal Health Care Finance Administration, which bears primary survey responsibility and can delegate survey and compliance monitoring to state or other health care jurisdictional authority. Institutional health care providers -- This group consists of hospitals, medical centers and clinics that currently comply with standards set by the Joint Commission on Accreditation of HealthcareOrganizations. Compliance to JCAHO standards enables institutional health care providers to obtain Medicare reimbursement for services to Medicare patients. The Medicare system is administered by the Federal Health Care Finance Administration, which bears primary survey responsibility and can delegate survey and compliance monitoring to state or other health care jurisdictional authority.
Caregivers typically invest six to nine months preparing for a JCAHO survey. The number of hours converted into dollars is considerable, not to mention cost to the institution for the actual survey. With ISO 9000 compliance, there is relatively little interruption in health care delivery as is experienced with the three-year JCAHO accreditation cycle.  Managed care and health maintenance organizations -- These groups experience similar problems when preparing for the National Committee for Quality Assurance HEDIS report card system. NCQA performs both accreditation and performance measurement. Although the standards differ from JCAHO's, the process is essentially the same, with a long lead time and significant preparation and survey costs. Managed care and health maintenance organizations -- These groups experience similar problems when preparing for the National Committee for Quality Assurance HEDIS report card system. NCQA performs both accreditation and performance measurement. Although the standards differ from JCAHO's, the process is essentially the same, with a long lead time and significant preparation and survey costs.
 Physician group practices -- This group can benefit from registration for two reasons. First, implementing ISO 9000 can create a more efficient practice, allowing physicians to identify problems and initiate corrective action quickly while also monitoring, controlling and reducing costs. Second, an ISO 9000-registered practice can point to its registration as a benchmark of an efficient and controlled operation. This is, more and more, what larger institutional provider organizations and insurance companies look for in terms of stable physician group practices. Physician group practices -- This group can benefit from registration for two reasons. First, implementing ISO 9000 can create a more efficient practice, allowing physicians to identify problems and initiate corrective action quickly while also monitoring, controlling and reducing costs. Second, an ISO 9000-registered practice can point to its registration as a benchmark of an efficient and controlled operation. This is, more and more, what larger institutional provider organizations and insurance companies look for in terms of stable physician group practices.
 Medical equipment service providers -- This group includes original equipment manufacturers, in-house biomedical engineering programs, independent service organizations and equipment remanufacturers. The U.S. Food and Drug Administration, which requires medical equipment manufacturers to comply with federal requirements known as good manufacturing practices, is petitioning for legislation requiring manufacturers to track equipment after sale. Given the large volume of medical equipment in use today as well as the equipment's portable nature, compliance would be virtually impossible. Medical equipment service providers -- This group includes original equipment manufacturers, in-house biomedical engineering programs, independent service organizations and equipment remanufacturers. The U.S. Food and Drug Administration, which requires medical equipment manufacturers to comply with federal requirements known as good manufacturing practices, is petitioning for legislation requiring manufacturers to track equipment after sale. Given the large volume of medical equipment in use today as well as the equipment's portable nature, compliance would be virtually impossible.
After receiving significant protests, the FDA has told equipment providers to implement a quality systems standard or be faced with GMPs or equivalent legislation. ISO 9000 can solve the problem with less impact on service costs than any other quality management system. Why ISO 9000? While ISO 9000 registration is notintended to replace JCAHO or NCQA accreditation, it does make the compliance-demonstration process appreciably less difficult, time-consuming and costly. The various health care organizations would adopt ISO 9000 standards for different needs. In its reference book The Memory Jogger 9000, GOAL/QPC lists the following reasons as common motivating factors for organizations:  To comply with customers who require ISO 9000 To comply with customers who require ISO 9000
 To compete in both domestic and international markets To compete in both domestic and international markets
 To improve existing quality systems To improve existing quality systems
 To minimize auditing by accrediting organizations To minimize auditing by accrediting organizations
 To improve subcontractors' and vendors' performances To improve subcontractors' and vendors' performances
With good planning, hard work and continuous improvement, health care providers and their organizations can use an ISO 9000 quality system to help them:  Achieve better understanding of quality practices throughout the organization Achieve better understanding of quality practices throughout the organization
 Ensure continued use of the required quality system Ensure continued use of the required quality system
 Improve documentation and records Improve documentation and records
 Strengthen both supplier and customer confidence and relationships Strengthen both supplier and customer confidence and relationships
 Gain cost savings and improve profitability Gain cost savings and improve profitability
 Form a foundation for ongoing total quality management Form a foundation for ongoing total quality management
However, complying with ISO 9000 standards doesn't ensure that every product or service meets customer requirements, only that the organization's quality system is capable of meeting them. To do that, organizations must continuously assess how satisfied customers are and improve the processes that create the products or services. ISO 9000 provides a quality management system that takes into account the measures, settings, services and functions of both clinical and administrative activities within the health care industry. ISO 9000-1 provides basic definitions and guidelines that can help health care providers select and use the appropriate standard. ISO 9001, ISO 9002 and ISO 9003 are system requirements, while ISO 9004-1 is a guideline. Policies, procedures, job instructions and documentation can be identified or created for each process and for each applicable clause within ISO 9001 or ISO 9002. ISO 9000 process improvement techniques Implementing ISO 9000 in all aspects of health care delivery requires unique approaches. Because the series is process-based rather than compliance-based, it's less complicated to implement than either of the JCAHO or NCQA/HEDIS accreditation systems. It is an excellent way to rationalize business processes in the health care industry. ISO 9000 works on the principle that an organization defines its own quality system based on processes that work best for it. Consequently, health care organizations interested in implementing ISO 9000 must first identify the health care measures in a given program as well as the setting in which health care is delivered and the services provided. The quality performance wheel concept described below provides a system for establishing goals for performance and improvement, program costs and customer satisfaction (see Figure 1). Any successful program must address all three topics. 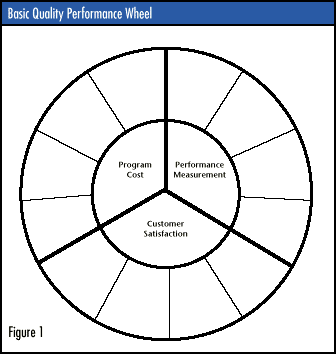 |
While quality management systems are well-established in the industrial environment, these concepts are, with a few exceptions, less than a decade old in the health care community. In addition, health care providers generally have had less training and/or experience in statistical and analytical tools, techniques and applications. Figure 4 demonstrates a tools flowchart coupled with problem-solving tools for use in identifying and solving problems while implementing ISO 9000. Health care services consist of many component parts, including institutional, ambulatory, long-term and home care; health care networks; and clinical laboratories. However, for each delivery mode, it's possible to identify measures for specific settings, services provided, clinical conditions, health function status, customer satisfaction, administrative functions and fiscal considerations. In addition to these component parts, health care professionals and managers often face a split focus regarding process and outcomes. Clinicians stress outcomes with less concern for how they arrived at them; managers, on the other hand, stress processes. It's possible for both process and outcome to work together, as demonstrated in Figure 5, the integrated health care quality management model used to implement ISO 9000. Getting everyone involved When implementing ISO 9000, every level of a health care organization contributes to the quality effort. Senior leaders participate in annual performance reviews, where they receive individual feedback from the board of trustees, employees and peers. Included in this evaluation aremeasures such as effectiveness in meeting short- and long-term strategic goals and communicating quality values to employees and other stakeholders. Senior leaders communicate and reinforce the organization's stakeholder focus and quality values to managers and supervisors. Communication methods can include job descriptions, bimonthly departmental and weekly individual meetings, and monthly reviews of a quality performance wheel. Departments also can identify subprocesses, customers, measurements and action plans that are aligned with performance and improvement. Stakeholder focus and quality values are communicated to the work force and reinforced through personnel policies, training, staff meetings, departmental meetings and newsletters. By means of a quality performance wheel, overall organizational and work unit quality as well as operational performance are reviewed monthly with department managers. An organizationwide sharing of quality knowledge should also be held monthly, during which individuals and/or teams report on their progress. The agenda might include progress reviews, recognizing team and individual efforts, correlating improvement efforts to the strategic plan and the quality wheel, and verifying organizational learning. Establishing goals and solving problems Quality performance wheels can be used to monitor and improve virtually any aspect of a health care delivery program or system. Figure 1 shows the basic performance wheel. The outer ring indicates the performance goal while the middle ring indicates minimum acceptable performance. This format can be used to develop performance goals for any quality management performance measurement and improvement consideration. Three key elements -- performance measurement, program cost and customer satisfaction -- represent the core for all programs. The object of the performance wheel is to move measurement goals from the minimum acceptable ring to the outer or performance goal ring, forming a perfect circle. The process is continuous because new goals can then be set that improve on past performance. The wheel displays system performance measures in relation to performance, which allows a balanced, comprehensive view of an organization's progress toward predetermined goals. These performance measures represent the top tier in a series of strategically important but increasingly specific documentation of process and outcome at the core process, department, work unit and individual levels. The performance wheel in Figure 2 shows measured and documented results of a recent survey and performance report for the JCAHO Environment of Care Standard. The inner circle includes seven key elements. Goals and minimum acceptable performance levels have been established. At least two target performance measures have been established for each of the seven key elements and are listed outside the outer ring. Figure 3 shows a hospital-based program. Statistical tools primarily identify causes of problems or situations. Analytical tools analyze and identify possible solutions to problems or situations that, for whatever reason, need to be corrected, changed or modified. Frequently the question arises over which tool is best suited to identify and solve a particular problem. Figure 4 shows 11 generally accepted steps of problem solving. The accompanying chart is then modified by adding the number for the appropriate step to the most appropriate statistical or analytical toolbox. Often, one of the tools can be used for problem solving and decision making. These analytical shortcuts have proved quite effective in the rapid but precise methodology of applied statistics in health care. Integrated health care quality management Figure 5 shows a quality management model for implementing ISO 9000. The model’s primary purpose takes into consideration both the process and outcome aspects of health care. Payers are beginning to show a preference for working with health care providers that provide information on process, or more specifically, the quality of treatment provided. For institutional and managed care providers, process is where most quality achievements can occur. Clinicians and direct health care providers, on the other hand, more often are concerned with outcomes. Strong support is growing on both sides to find ways to improve both process and outcome without compromising either. The integrated health care quality management model depicts a method for implementing ISO 9000 as both process quality management and outcome quality management. Both sides share the fundamental reasons for more quality management in health care, which are:  Increased public demand for performance data in health care delivery Increased public demand for performance data in health care delivery
 Potential decline in financial resources that would affect the quality of medical care Potential decline in financial resources that would affect the quality of medical care
 Lack of sufficient evidence to support the effectiveness and reliability of many diagnostic and therapeutic methods Lack of sufficient evidence to support the effectiveness and reliability of many diagnostic and therapeutic methods
 Competition among providers for payer purchases of health care Competition among providers for payer purchases of health care
 Financial concerns of third parties Financial concerns of third parties
ISO 9000 has been used successfully to address similar issues in industry, at both manufacturing and management levels. With many established models already in place, the health care industry can apply the garnered knowledge to its own challenges and look forward optimistically to the benefits of this adaptable standard within the various fields of caregiving. About the author David A. Simmons, Sc.D., P.E., CCE, directs the health care division of Alamo Learning Systems, a training and consulting firm that specializes in assisting health care organizations to register to ISO 9000 utilizing Alamo’s Fast Track process. He is chair-elect of ASQ’s health care division. Simmons’ numerous publications include Medical and Hospital Control Systems and the Clinical Engineering Manual. Currently in production are Quality Management for Health Care and ISO 9000 for Health Care. He can be reached at telephone (800) 829-8081 or e-mail dsimmons@qualitydigest.com. |

