Every Wednesday We Scramble for Beds
 In my work, I visit a lot of hospitals. Right now, because of intense cost pressures, bed space is at a premium. From a lean perspective, you want a bed available for a patient exactly when needed, and you want the patient to stay only as long as needed. It’s a hospital version of just-in-time, and issues of flow are critical, as is predicting how many patients to expect. In my work, I visit a lot of hospitals. Right now, because of intense cost pressures, bed space is at a premium. From a lean perspective, you want a bed available for a patient exactly when needed, and you want the patient to stay only as long as needed. It’s a hospital version of just-in-time, and issues of flow are critical, as is predicting how many patients to expect.
A hospital that faced chaos related to this issue every Wednesday shared a year’s worth of its daily data regarding admits—which were made up of elective (planned) and acute (unplanned, on demand)—and discharges.
As part of a preliminary perusal of this data, I created a measure of overall “flow” (i.e., daily overall admits minus daily discharges) and looked at it separately for each day of the week.
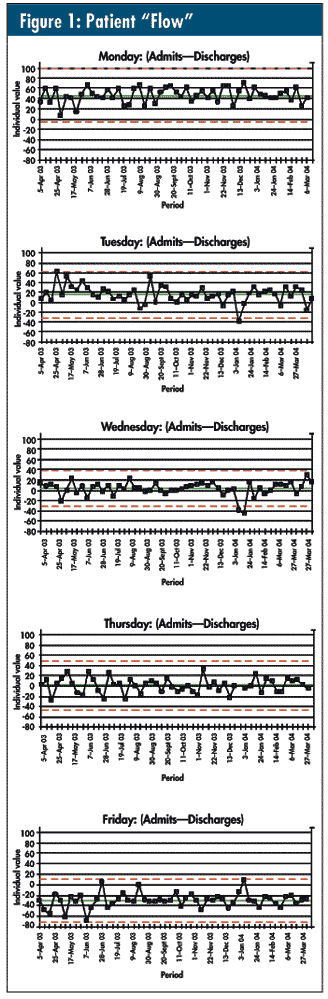
Leaving weekends aside (allowing for the fact that most elective surgery is done during the week), my jaw dropped when I saw the control charts in figure 1 by weekday. Look at the remarkable stability—and look, also, at the variability!
Note Monday’s and Tuesday’s averages—46 and 16, respectively. From this cursory analysis, it would seem that, by the end of Tuesday, the hospital has 62 more beds occupied than at the beginning of Monday. Note that Wednesday seems to balance admits and discharges (an average of zero) and shows one-third less variation. On Friday, a notoriously low surgery day, the hospital is finally able to alleviate the alleged overcrowding by discharging 30 more patients than are admitted. This is what happens—on average.
However, consider the variation: ±50–55 on Monday and Tuesday, ±35 on Wednesday and ±40–50 on Thursday and Friday. Is it any wonder that Wednesdays seemed so chaotic? However, as shown by the control charts, the system is perfectly designed for this to happen. Furthermore, by treating every Wednesday as a special cause when it’s obviously a common cause, the administrators haven’t improved the situation. In fact, they could very well be making it worse.
Their reaction when I presented them with this? “That can’t be true because it’s not supposed to be like that.”
Maybe it wasn’t “supposed” to happen, but the data don’t lie. Such incredible variation points to the culprit: The system is incapable of flow.
The most common reaction to the problems it created was to cancel surgeries to create beds. When the “unplanned” admissions were analyzed, they were perfectly predictable (virtually classic Poisson counts). Even though there were almost half as many elective admissions, they were twice as variable as the unplanned because of this overreaction (or tampering), which created even more chaos.
First and foremost, there must be coordination between admissions and discharges for better prediction of the number of patients—and types of patients—and the system’s capability to absorb natural peaks. Typically, theory says that one should have 20-percent excess beds, which throws hospitals into a panic because, in my experience, most of them operate at close to 100-percent capacity; 20 percent over and above that would be cost-
prohibitive. Actually, rather than add beds, this hospital needs to reduce its flow variation so that the current 100-percent point becomes the 20-percent excess point.
It’s not about reducing costs but, rather, reducing four other Cs—confusion, complexity, conflict and chaos.
Davis Balestracci is a degreed statistician and consultant well-known for “waking up” conferences with his passionate public speaking. Visit his Web site at www.dbharmony.com.
|